Chronic disease management is a vital component of modern healthcare, emphasizing a systematic approach to dealing with long-term health conditions. It involves collaboration among healthcare professionals, patients, and caregivers to enhance the quality of life and health outcomes for those affected by chronic illnesses. With the growing prevalence of chronic diseases, understanding their management becomes increasingly crucial for fostering healthier communities and informed patients.
Effective strategies for chronic disease management include developing personalized care plans, leveraging technology for monitoring, and empowering patients through education. These techniques not only improve adherence to treatment but also address the various challenges associated with chronic health conditions.
Chronic Disease Management Overview
Chronic disease management is a comprehensive approach aimed at improving the quality of life for individuals living with long-term health conditions. It encompasses a range of strategies and interventions designed to prevent disease progression, manage symptoms, and enhance patient engagement in their own care. Given the rising prevalence of chronic diseases worldwide, effective management is crucial not only for individual well-being but also for the sustainability of healthcare systems.Healthcare professionals play a pivotal role in chronic disease management, acting as coordinators, educators, and support systems for patients.
Their responsibilities often include creating personalized care plans, monitoring patient progress, and providing necessary education regarding lifestyle modifications. This multidisciplinary approach involves various healthcare providers, including primary care physicians, nurses, dietitians, and pharmacists, all working together to optimize patient outcomes.
Common Chronic Diseases and Their Impact
Chronic diseases encompass a wide range of health conditions that often require ongoing medical attention and can limit daily activities. The impact of these diseases on patients’ lives is profound, affecting not only physical health but also emotional and social well-being. The following are some of the most common chronic diseases and their implications:
- Diabetes: Affects more than 463 million people globally and can lead to severe complications such as heart disease, kidney failure, and limb amputation if not managed properly.
- Hypertension: Often referred to as a “silent killer,” it increases the risk of stroke and heart attack, impacting daily activities and requiring lifelong management.
- Asthma: Affects millions of individuals, causing difficulty in breathing and requiring continuous management to minimize exacerbations that can lead to hospitalizations.
- Chronic Obstructive Pulmonary Disease (COPD): Significantly impacts lung function, leading to limitations in physical activity and a decreased quality of life, with a notable increase in healthcare costs.
- Heart Disease: Remains a leading cause of death globally, affecting the heart’s ability to function effectively and often requiring regular monitoring and medication adherence.
The management of these chronic conditions typically involves a combination of medication, lifestyle changes, and regular monitoring. For instance, individuals with diabetes need to regularly check their blood sugar levels, follow a diet plan, and maintain a consistent exercise regimen. These interventions can significantly reduce complications and improve overall health outcomes.
“Effective chronic disease management not only enhances patient quality of life but also reduces healthcare costs associated with disease progression.”
Through early intervention and ongoing support, healthcare professionals can help patients navigate the complexities of chronic disease management, ensuring they remain engaged and informed about their health choices.
Strategies for Effective Chronic Disease Management
Chronic disease management requires a multifaceted approach that addresses the unique needs of each patient. Implementing effective strategies can significantly improve patient outcomes and enhance their quality of life. Understanding personalized care plans, the role of technology, and patient education techniques are crucial in this endeavor.
Personalized Care Plans for Chronic Disease Patients
Creating personalized care plans is essential in addressing the specific needs of chronic disease patients. These plans should be tailored based on individual health profiles, preferences, and life circumstances. The following components are critical in developing an effective personalized care plan:
- Comprehensive Assessment: Start with a thorough evaluation of the patient’s medical history, current health status, and lifestyle factors. This assessment forms the basis for the care plan.
- Goal Setting: Collaborate with the patient to establish realistic health goals. These could include improving medication adherence, managing blood sugar levels, or increasing physical activity.
- Interdisciplinary Collaboration: Ensure that the care plan involves a team of healthcare providers, including doctors, nurses, dietitians, and social workers, to address all aspects of the patient’s care.
- Regular Review and Adjustment: Schedule regular follow-ups to assess progress and make necessary adjustments to the care plan based on the patient’s evolving needs.
Role of Technology in Monitoring Chronic Conditions
Technology plays a pivotal role in the management of chronic diseases by facilitating continuous monitoring and communication. Various technological tools can enhance patient care and improve health outcomes:
- Wearable Devices: Gadgets such as smartwatches and fitness trackers can monitor vital signs, physical activity, and sleep patterns. For example, devices like the Fitbit can provide real-time feedback to users regarding their activity levels.
- Mobile Health Apps: Applications designed for chronic disease management exist to help patients track medication adherence, schedule appointments, and log symptoms. Apps like MySugr for diabetes encourage patients to engage actively in their health.
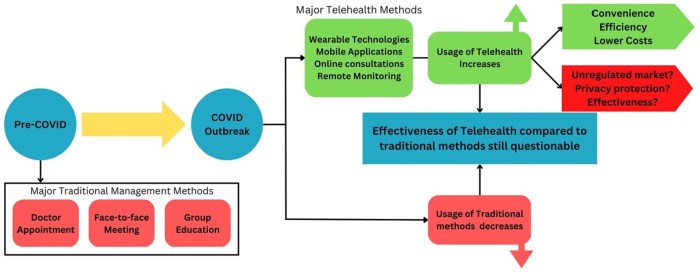
- Telehealth Services: Virtual consultations allow healthcare providers to monitor patients remotely, which is particularly beneficial for those with mobility issues or those living in rural areas.
- Data Analytics: Utilizing data collected from various sources can facilitate predictive analytics to identify potential health risks before they escalate into serious issues.
Patient Education Techniques for Empowerment
Empowering patients with knowledge about their conditions is crucial for effective chronic disease management. Educated patients are more likely to engage in their care and make informed decisions. Effective education techniques include:
- Interactive Workshops: Conduct workshops that allow patients to learn about their chronic conditions in a collaborative environment, fostering peer support and shared experiences.
- Personalized Educational Materials: Create tailored educational resources that address the specific needs and literacy levels of the patients, making the information accessible and relatable.
- Motivational Interviewing: Utilize motivational interviewing techniques to help patients explore their own motivations and enhance their commitment to following their care plans.
- Regular Feedback Mechanisms: Provide opportunities for patients to ask questions and give feedback on their treatment, ensuring they feel heard and involved in their care process.
Empowering patients through education and technology not only enhances their self-management abilities but also fosters a more collaborative relationship with healthcare providers.
The Intersection of Dentistry and Chronic Disease Management

Oral health is a crucial, yet often overlooked, component of chronic disease management. The connection between the mouth and the rest of the body has been increasingly recognized in recent years, illustrating the significant role dental professionals play in supporting overall health. By addressing oral health, we can positively impact the management of various chronic diseases, leading to better health outcomes for patients.The relationship between oral health and chronic diseases is multifaceted.
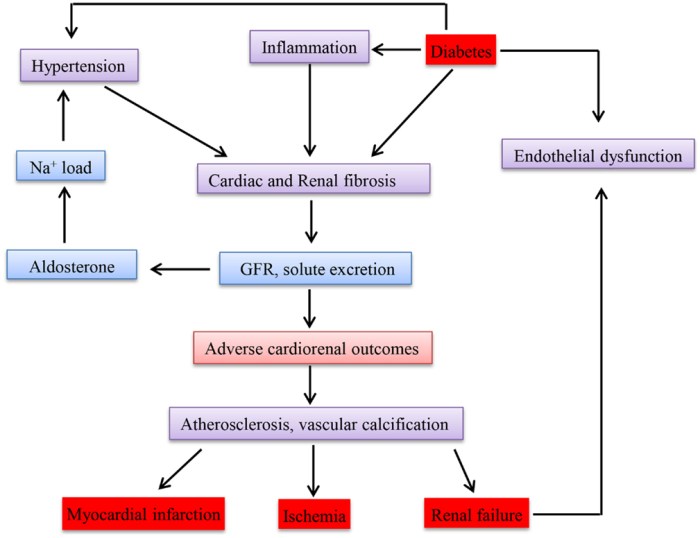
Conditions such as diabetes, heart disease, and respiratory illnesses have been linked to poor oral health. For instance, individuals with diabetes are more susceptible to gum disease, while those with periodontal disease may experience difficulties in blood sugar control. This bi-directional relationship emphasizes the need for integration between dental care and chronic disease management, as neglecting oral health can exacerbate these chronic conditions.
Role of Dental Professionals in Chronic Disease Management
Dental professionals can significantly contribute to chronic disease management through early detection, education, and collaborative care. They are in a unique position to assess oral health, which can reflect systemic health issues. Here are some ways dental professionals can engage in chronic disease management:
- Screening for Chronic Conditions: Dentists can identify signs of diseases such as diabetes and heart disease during routine dental examinations. Early detection allows for timely referrals and interventions.
- Patient Education: Educating patients about the importance of oral hygiene can help reduce the risk of developing chronic diseases. Providing resources and strategies for effective oral care can empower patients to take charge of their health.
- Interdisciplinary Collaboration: By working with medical professionals, dental practitioners can coordinate care plans that address both oral and systemic health needs, fostering a holistic approach to patient care.
- Monitoring Oral Health: Regular dental visits can help monitor changes in oral health that may indicate worsening chronic conditions, allowing for prompt action to be taken.
Challenges and Solutions in Integrating Dental Care
Despite the clear connection between oral health and chronic diseases, there are several challenges in integrating dental care into chronic disease management practices. These challenges include:
- Lack of Awareness: Many healthcare providers may not fully recognize the link between oral health and chronic diseases. This gap can lead to missed opportunities for early diagnosis and intervention.
- Fragmented Care Systems: The separation between dental and medical care often results in fragmented treatment plans. Patients may find it difficult to navigate between different healthcare providers, leading to inadequate care coordination.
- Limited Training: Dental professionals may not receive extensive training on how to manage chronic diseases, which can hinder their ability to provide comprehensive patient care.
To address these challenges, several solutions can be implemented:
- Education and Training: Providing dental professionals with education on chronic disease management can enhance their ability to participate in integrated care approaches.
- Developing Collaborative Models: Creating models of care that encourage collaboration between dental and medical professionals can improve patient outcomes and streamline care delivery.
- Increasing Public Awareness: Campaigns to inform both patients and healthcare providers about the importance of oral health in chronic disease management can foster proactive health behaviors.
In summary, the intersection of dentistry and chronic disease management showcases the vital role oral health plays in overall well-being. Through collaboration, education, and a commitment to integrated care, dental professionals can help bridge the gap between oral and systemic health, ultimately enhancing patient care and improving health outcomes.
Epilogue
In summary, chronic disease management is an essential aspect of healthcare that requires a multi-faceted approach involving various stakeholders. By understanding the interaction between chronic diseases and overall health, especially the role of oral health, we can create a more integrated care model that enhances patient outcomes. Emphasizing preventive measures and continuous education will further equip individuals to navigate their health journeys successfully.
FAQ Resource
What is chronic disease management?
Chronic disease management refers to the organized, multidisciplinary approach to managing long-term health conditions to improve patient outcomes and quality of life.
Who is involved in chronic disease management?
Healthcare professionals, including doctors, nurses, dietitians, and pharmacists, work together to create and implement care plans for patients with chronic diseases.
How does technology aid in chronic disease management?
Technology provides tools for remote monitoring, data collection, and communication, allowing for timely interventions and better adherence to treatment plans.
Why is patient education important in this context?
Patient education empowers individuals by equipping them with knowledge and skills to manage their conditions effectively, leading to improved health outcomes.
What are common challenges in chronic disease management?
Challenges include ensuring patient adherence to treatment, coordinating care among multiple providers, and addressing the psychological aspects of chronic illnesses.